Symptoms, Causes, and Treatments
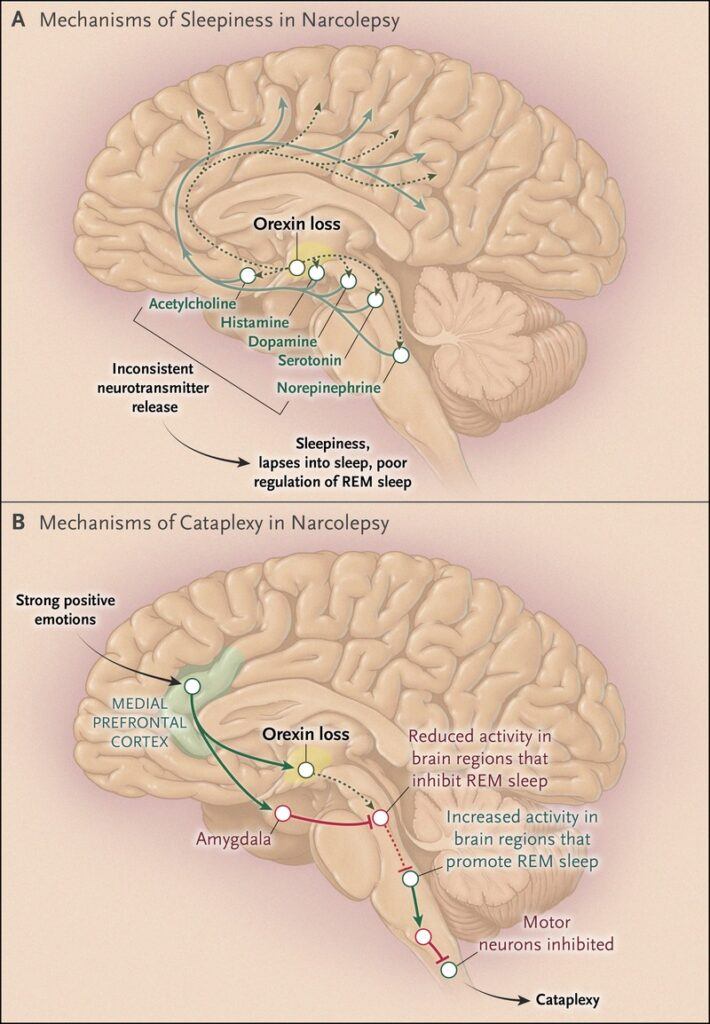
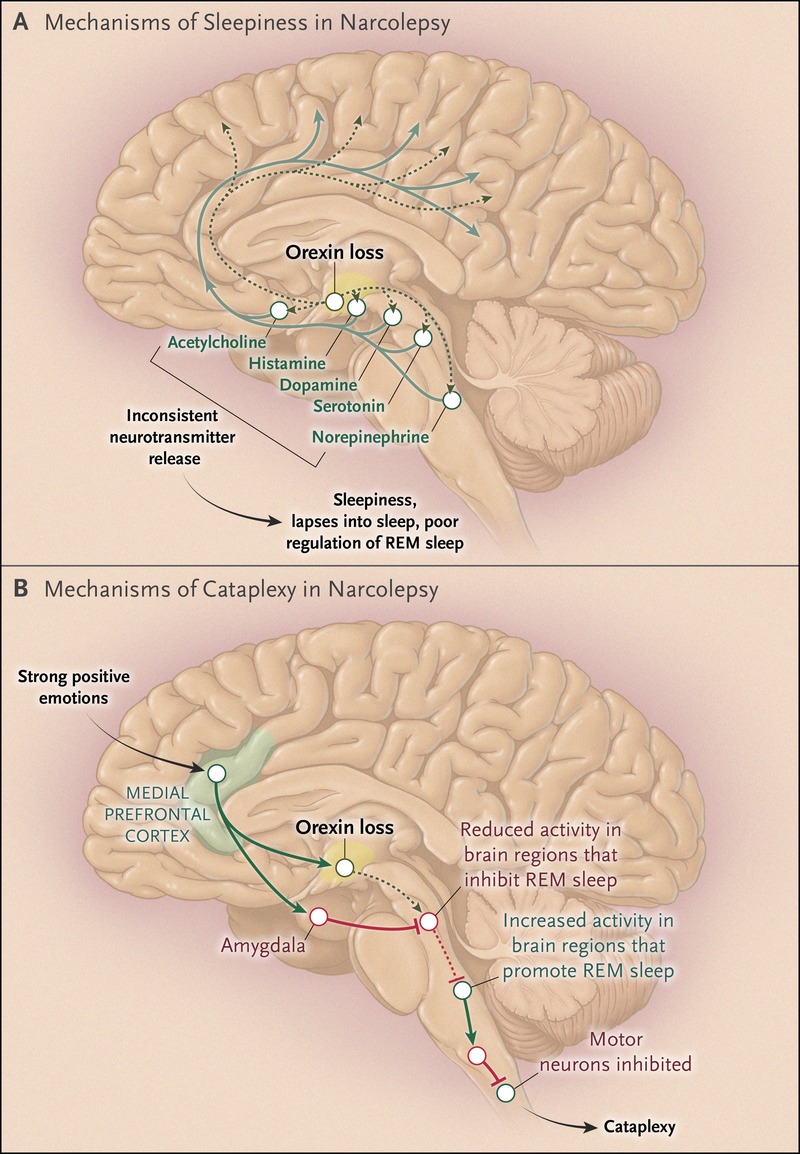
Narcolepsy is a chronic sleep disorder characterized by overwhelming daytime drowsiness and sudden sleep attacks. It disrupts the brain’s ability to regulate sleep-wake cycles, often leading to severe disruptions in daily life, work, and social relationships. Although narcolepsy can be a serious condition, it is generally manageable with proper treatment and care.
Symptoms and Causes
Symptoms of Narcolepsy:
- Excessive Daytime Sleepiness (EDS):
- EDS is the hallmark of narcolepsy, leading to uncontrollable urges to sleep during the day, often referred to as “sleep attacks.”
- Cataplexy:
- Sudden loss of muscle tone triggered by strong emotions such as laughter or anger. This can range from mild weakness to complete body collapse.
- Sleep Paralysis:
- Temporary inability to move or speak while falling asleep or waking up, often accompanied by vivid and frightening hallucinations.
- Hallucinations:
- Vivid and often frightening visual or auditory experiences that occur at the onset of sleep (hypnagogic) or upon waking (hypnopompic).
- Other Symptoms:
- Automatic behaviors (performing tasks without conscious awareness)
- Memory problems and forgetfulness
- Sudden outbursts or unusual verbal expressions during sleep attacks
Types of Narcolepsy:
- Type 1:
- Includes cataplexy and low levels of orexin (hypocretin), a brain chemical that regulates wakefulness.
- Type 2:
- Does not involve cataplexy, and the exact cause is less understood.
Causes:
- Type 1 Narcolepsy:
- Often linked to an autoimmune response that reduces orexin levels.
- Type 2 Narcolepsy:
- Less clear but may involve orexin signaling or other unknown factors.
- Secondary Narcolepsy:
- Resulting from brain injuries or genetic conditions.
Diagnosis and Tests
Diagnosing narcolepsy involves multiple steps to rule out other conditions and confirm the presence of specific symptoms.
Diagnostic Tests:
- Polysomnogram (PSG):
- An overnight sleep study that records brain waves, blood oxygen levels, heart rate, and breathing.
- Multiple Sleep Latency Test (MSLT):
- Measures how quickly you fall asleep during the day in a quiet environment.
- Maintenance of Wakefulness Test (MWT):
- Assesses the ability to stay awake for a defined period in a quiet, non-stimulating environment.
- Spinal Tap (Lumbar Puncture):
- May be performed to measure orexin levels in the cerebrospinal fluid, particularly in cases of Type 1 narcolepsy.
Management and Treatment
While there is no cure for narcolepsy, several treatments can help manage symptoms and improve quality of life.
Medications:
- Wakefulness-Promoting Agents:
- Modafinil and armodafinil help reduce daytime sleepiness.
- Stimulants:
- Methylphenidate and amphetamines may be prescribed to maintain wakefulness.
- Antidepressants:
- SSRIs, SNRIs, and tricyclic antidepressants can help manage cataplexy and other REM sleep-related symptoms.
- Sodium Oxidate:
- A powerful medication that helps with both nighttime sleep and cataplexy.
- Histamine-Affecting Drugs:
- Pitolisant is another option for reducing daytime sleepiness.
Lifestyle Adjustments:
- Scheduled Naps:
- Incorporating short naps into the daily routine can help manage daytime sleepiness.
- Good Sleep Hygiene:
- Maintaining a regular sleep schedule and creating a restful environment.
- Diet and Exercise:
- Regular physical activity and a balanced diet can improve overall sleep quality.
Prevention
While narcolepsy cannot be prevented, early diagnosis and treatment can help manage symptoms effectively. Educating yourself and others about the condition can also reduce stigma and improve support.
Outlook/Prognosis
With proper treatment and lifestyle adjustments, individuals with narcolepsy can lead fulfilling lives. Ongoing management and regular follow-ups with healthcare providers are crucial for optimal outcomes.
Living With Narcolepsy
Living with narcolepsy requires adaptability and support. Joining support groups, seeking professional counseling, and educating family and friends can enhance coping strategies and improve quality of life. It’s essential to work closely with healthcare providers to tailor a treatment plan that addresses individual needs and promotes overall well-being.
Narcolepsy may be a lifelong condition, but with the right care, it is manageable. Stay informed, seek support, and prioritize your health to navigate the challenges and live a fulfilling life.
Conclusion
Narcolepsy is a serious but manageable condition. Proper diagnosis, treatment, and lifestyle adjustments can significantly improve the quality of life for those affected. By understanding the symptoms, causes, and available treatments, individuals with narcolepsy can better manage their condition and lead fulfilling lives.
Incorporating this information into your daily routine and staying informed about new treatments and research can help you take control of your narcolepsy and live a healthier, more balanced life.
This article is not meant to treat or cure any health issues. It is informational only. As always, seek help from a professional Health Care provider before taking any medications or attempting any unsupervised treatments.